Clinical reasoning for sensory processing is essential for professionals working with children, yet translating sensory theory into effective practice can be challenging. Many therapists, educators, and clinicians understand that sensory processing influences behavior, learning, and participation – but knowing the theory and applying it meaningfully in everyday environments are two very different things.
This was a key theme explored during the Sensory Summit 2025, where we discussed how clinicians can strengthen their clinical reasoning and move beyond surface-level sensory support.
In many therapy and classroom settings, sensory strategies can unintentionally become routine or generic. Interventions may rely on familiar tools such as fidget toys, obstacle courses, or sensory bins. While these activities can certainly be helpful, they do not automatically address the underlying sensory needs of a child.
To truly support children’s development and participation, we need to move beyond generic sensory activities and instead unpack sensory needs one child at a time, using thoughtful observation, structured frameworks, and strong clinical reasoning.
Why Sensory Clinical Reasoning Matters
Sensory processing differences are often invisible. What we observe as therapists, educators, or clinicians is the child’s outward behavior or performance. But behavior is only the surface.
When a child struggles in a particular situation, our role is to ask a deeper question: What might be happening underneath?
Take a common example: a child avoiding circle time.
At first glance, it might appear that the child is disengaged or refusing to participate. However, many underlying factors could be contributing to this behavior.
The child may be struggling with:
- Postural control – sitting on the floor may be physically challenging
- Vestibular processing – getting up and down from the carpet may feel disorienting
- Auditory input – noise from other children can be overwhelming
- Language processing – the pace of conversation may be difficult to follow
- Tactile sensitivity – the texture of the carpet may be uncomfortable
- Executive functioning – sequencing and maintaining attention may be demanding
Too often, we apply broad labels such as “behavioral” or even simply “sensory.” But these labels rarely tell us what the child actually needs.
This is where clinical reasoning becomes essential.
The Pyramid of Learning: Understanding the Foundations of Behavior
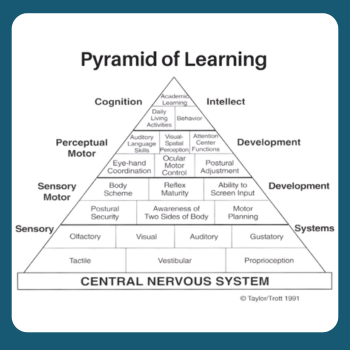
One framework I often use when supporting clinical reasoning is the Pyramid of Learning, developed by Kathleen Taylor, an occupational therapist, and Maryann Trott, a special educator.
This model helps explain how foundational sensory and motor systems support higher-level learning and behavior.
The pyramid consists of four key layers.
1. The bottom layer is the Central Nervous System – the neurological foundation that supports all development.
2. Then we have the Sensory Systems and Sensory Motor Development – this layer includes: body awareness, reflex integration, motor planning, balance and movement
3. The third layer is Perceptual-Motor Development – this includes skills such as: visual-spatial perception, auditory processing and oculomotor control.
4. And at the top of the pyramid is Cognition and Intellect – this is our behavior and academic learning.
The purpose of Taylor and Trott’s Pyramid of Learning is to give therapists, teachers, and parents a visual tool for explaining why sensory processing or motor skills really matter. If the foundations at the bottom of the pyramid are not well supported, it will impact the skills at the top. This is why focusing only on behavior or academic skills may miss the underlying challenges affecting a child’s ability to participate.
What Sensory Integration Is (and Is Not)
When discussing sensory processing, there are several common misconceptions about sensory therapy that are important to address.
➜ Sensory integration is not aversive exposure
Sensory integration therapy is sometimes confused with approaches that repeatedly expose a child to uncomfortable stimuli in order to force tolerance.
For example, asking a child with tactile sensitivity to repeatedly place their hands into unpleasant textures in order to “desensitize” them. This approach does not reflect sensory integration principles.
➜ Sensory integration is not generic sensory stimulation
Another misconception is that sensory input alone is therapeutic.
Providing the same sensory activities to every child – such as identical sensory diets or predetermined movement breaks – lacks the clinical reasoning necessary for meaningful intervention.
While all children benefit from movement, outdoor play, and rich sensory experiences, these are examples of health promotion, not individualized sensory integration therapy.
➜ Sensory integration is not just sensory-motor activities
Obstacle courses, movement games, and sensory-motor groups can be incredibly beneficial for children. However, simply running sensory-motor activities does not mean that a child’s sensory processing needs are being addressed.
The key question should always be: Why this activity, for this child, at this moment?
Understanding Sensory Integration
The theory of Sensory Integration Theory was developed by A. Jean Ayres, an occupational therapist who closely observed how children learn and participate in everyday activities.
Through her work, Ayres noticed that some children struggled in school not because of their intelligence, but because of how their brains processed and organized sensory information. These children often had difficulty responding to the sensory demands of their environments, which affected their ability to engage in learning, play, and daily routines.
Ayres described sensory integration as the organization of sensations for use – the brain’s ability to receive, interpret, and integrate sensory information so that we can respond effectively to the world around us.
To support both assessment and research in this area, Ayres also developed the Sensory Integration and Praxis Tests (SIPT) a comprehensive tool designed to measure sensory integration and praxis (motor planning).
She captured the experience of sensory processing challenges with the following metaphor: “When the flow of sensation is disorganized, life can feel like a rush hour traffic jam.” (Ayres, 1979)
This concept highlights how difficulties in organizing sensory input can affect a child’s ability to produce adaptive responses and participate successfully in everyday environments.
Brain Plasticity and Adaptive Responses
A central concept in sensory integration is brain plasticity – the brain’s ability to change through experience.
One way to imagine this is to think of the brain as a field of tall grass. Each time a child practices a skill or interacts with their environment, they create a pathway through the grass. Over time, these repeated experiences strengthen those neural pathways.
Through play, exploration, and carefully designed therapeutic environments, children can develop adaptive responses – goal-directed actions that help them interact successfully with the world around them.
Key Sensory Processing Processes
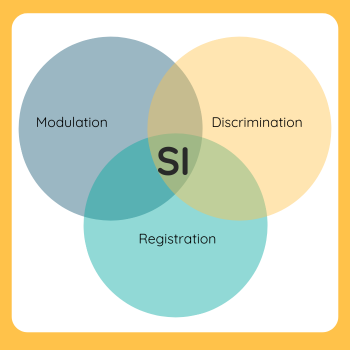
Effective sensory integration relies on three important processes.
Registration: This is the detection of sensory input like noticing a pencil in your hand, hearing a bell ring or feeling heat from a surface.
Modulation: Modulation refers to adjusting responses to the intensity and duration of sensory input. This process plays a major role in emotional and behavioral regulation.
Discrimination: Discrimination involves interpreting sensory details and using past experiences to guide action. For example, knowing how much force to use when hitting a baseball based on previous attempts.
When these processes work together effectively, the result is an adaptive response – a meaningful and appropriate reaction to sensory input.
Sensory Processing Patterns in Daily Life
Another important perspective comes from Winnie Dunn, who developed Dunn’s Sensory Processing Framework. While Ayres’ work focuses on intervention and building adaptive responses, Dunn’s framework helps describe how children respond to sensory input in everyday environments.
Dunn’s model is based on two key concepts: neurological thresholds and self-regulation strategies. A neurological threshold refers to how much sensory input a child needs before their nervous system registers it. Children with a high threshold require more sensory input before noticing it, while those with a low threshold detect sensory input quickly and may become overwhelmed more easily.
The second concept describes how children respond to sensory input. Some use active strategies, such as seeking or avoiding sensory experiences, while others respond passively, allowing the sensory environment to affect them.
When these two factors combine, they create four sensory processing patterns: low registration, sensation seeking, sensory sensitivity, and sensation avoiding. Understanding these patterns helps clinicians interpret children’s responses to sensory environments and design more supportive accommodations and strategies.
Bringing It All Together: A Clinical Reasoning Framework
When supporting children with sensory processing differences, I find it helpful to follow a structured clinical reasoning process. Rather than jumping straight to strategies, the goal is first to understand what we are observing and why it may be happening.
The process begins by describing the behavior objectively, without interpretation. For example, we might note that a child leaves circle time, refuses to use the swing, or has meltdowns during transitions. From there, it is important to examine the environmental context, including factors such as noise levels, lighting, physical space, and the demands of the activity, as these can significantly influence how a child experiences a situation.
I also consider personal factors that may be affecting the child in the moment, such as fatigue, hunger, anxiety, or unfamiliar settings. These elements can amplify sensory challenges or make otherwise manageable situations more difficult.
Next, I refer back to the Pyramid of Learning, looking “down the pyramid” to identify which underlying systems may be contributing to the difficulty. While the behavior appears at the top, the root cause may lie in foundational areas such as sensory processing, motor planning, posture and balance, perceptual processing, or executive functioning.
At this stage, I generate a working hypothesis. In some cases, Dunn’s Sensory Processing Framework may help explain a child’s sensory thresholds and regulation patterns, guiding environmental supports. In other cases, the challenge may align more closely with Ayres Sensory Integration, suggesting that therapy should focus on developing new adaptive responses.
This hypothesis can then be tested through assessment and observation, drawing on standardized tools, clinical observations across contexts, and insights from parents, teachers, and other team members. Once the reasoning becomes clearer, interventions can be aligned with the child’s needs, whether through environmental adaptations, compensatory supports, or child-led sensory integration therapy.
Using a structured reasoning process helps move us away from trial-and-error strategies and toward interventions that are intentional, individualized, and grounded in sensory theory.
Sensory Processing Is Everyone’s Responsibility
There is a common misconception that sensory processing is the domain of occupational therapists alone. In reality, sensory processing sits at the foundation of the learning pyramid, meaning it influences many aspects of development.
Professionals across disciplines encounter sensory processing every day:
- Occupational Therapists integrate sensory strategies with goals in self-care, play, school participation, and emotional regulation.
- Speech-language Pathologists frequently encounter children whose communication and feeding are impacted by sensory processing differences; understanding sensory frameworks allows SLPs to interpret assessments collaboratively with OTPs and optimize the child’s environment.
- Physical Therapists encounter sensory processing through balance, posture, gait, and motor planning, since sensory differences directly influence these motor outputs.
- Educators and early childhood professionals see sensory needs in the classroom and can implement accommodations or supports to help children participate successfully.
While each discipline may address sensory processing differently, a shared understanding of sensory frameworks allows teams to better support children’s participation across environments.
So to tie it all together…
Behavior is often the visible surface of deeper sensory and neurological processes. By strengthening our clinical reasoning and drawing on frameworks such as the Pyramid of Learning, Ayres Sensory Integration, and Dunn’s Sensory Processing Model, we can move beyond generic sensory activities and develop interventions that truly meet a child’s needs.
When we take the time to understand what is happening beneath the surface, we create more supportive environments, more effective interventions, and ultimately better outcomes for children.
This is just a glimpse: get the full presentation plus 11 other expert-led talks on moving beyond surface-level sensory strategies, and unpacking sensory needs – one case at a time